This page will give you some deeper information about the materials that are used for smile makeovers and porcelain veneers. Some data may be very technical or may remind you of a chemistry class. However, many of these materials remain in your mouth for many, many years. It is therefore up to you to decide whether you want to know about them.
- Dental Bonding Agents
- Cements
- IPS Empress and Emax Porcelains
- Porcelain Fused to Metal
- What are Porcelains?
- Dental Composites
Dental Bonding Agents

The seepage of fluid to the tooth surface is caused be positive pressure of the pulp of the tooth. Acetone-based materials are less influenced by dentinal fluid, which lowers the bond strength of alcohol or water-based bonding agents.
There are many other bonding agents available and new ones are regularly released by dental-product developing companies. However, it is most important that the cosmetic dentist understands the structural biology of the tooth surface and the chemistry of his favorite bonding system. This will ensure that the agent is applied using proper technique as required by the individual chemistry of the product and its specific interaction with the tooth surface. Research has shown that problems arising from improper handling of the bonding agents pose much greater problems than the lack of an inherent bond strength of a particular dental bonding system.
Two other popular fourth-generation bonding systems are OptiBond FL, which has been show to obtain bond strengths of up to 39 MPa (Cristensen GJ, 2010) and Scotchbond MP, which has demonstrated bond strengths of up to 45.6 MPa (DeMunck J, 2003).
Later generations of bonding systems have been developed. However, they are not any better than the fourth-generation bonding systems, just easier to use. This has been achieved by combining the steps etch-prime-adhesive into one bottle. A recent study has shown that All Bond 2 is still the gold standard leading to better bonding strengths than these new systems. Melo RM et al, 2010, have shown that All Bond 2 led to up to 44 MPa as opposed to self-etch systems that only led to bond strengths of up to 26 MPa. This appears to make sense since this author believes that mobilized molecules from acid treatment need to be rinsed away to provide a deeper retentive pattern and more patent paths for the hydrophilic primer to percolate.
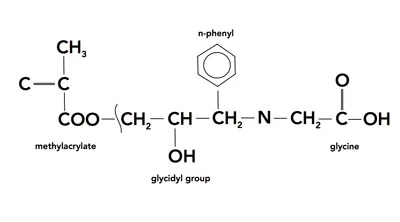
A one to one mix of All Bond 2 Primers A and B is very versatile. It binds to all substrates and efficiently seals dentinal tubules, which help prevent dentinal sensitivity. Primer A contains NTG-GMA. Primer B contains BPDM, which leads to high bonding strengths. D/E Resin is a light-cured unfilled resin.
Scotchbond Universal is a single-component bonding agent. It can be used in total-etch procedures. It contains MDP and silane, which makes a separate silanation of the intaglio surfaces of porcelain veneers unnecessary. It is ethanol based and . It is best used with the luting cement RelyX Ultimate, which makes the use of a dual-cure activator unnecessary.
Scotchbond Universal is applied immediately, after treatment of the prepared tooth surface with a phosphoric acid etching ge,l to the entire surface of the enamel and dentin and rubbed in for 20 sec. Subsequently a gentle stream of air is directed over the liquid layer for about 5 sec until it no longer moves. Now the solventhas evaporated. For this specific application of luting porcelain veneers with RelyX Veneer Cement, the dried Scotchbond Universal layer is not light-cured.
The veneer is etched with hydrofluoric acid and apply Scotchbond the same way as on the prepared tooth structure. It is not light-cured either.
Cements
The cements used to bond the restorative materials to the conditioned tooth surface are filled resin cements (mostly so-called hybrids). We use a dual-cure resin cement, which means that it sets both by its own catalyst and through activation with monochromatic light. It is available in six shades. It is filled to 68% with pre-polymerized micro-particles of different sizes (hybrid), which minimizes the polymerization shrinkage that is common with resins.
We also use a phosphate-ester adhesive resin cement that doesn't need to be cured with light. The great variety of resin cements makes it difficult for the clinician to clearly make a material selection based on scientific evidence. It is therefore important to become familiar with the chemistry and technical requirements of only a few materials and to gain experience.
My favorite luting cements for porcelain veneers are Variolink Esthetic LC and RelyX Veneer Cement. They are purely light cured and color stable. Their working time and can be fully controlled per preferences of the treating cosmetic dentist.
RelyX Veneer Cement contains silane-treated cermic and silica as fillers, as well as reacted polycaprolactone polymer and titanium dioxide among other ingrediences, whose exact proportions in the composition are trade secrets. It contains a high efficiency photoinitiator which makes the cement to cure more quickly than many of the other cements available. It is free of aromatic amine components to ensure color stability.
Variolonk Esthetic LC is the successor of Variolink II. It is also shade stabile due to the reactive light initiator Ivocerin which is 100% amine-free. It displays lifelike fluorescence and is radioopaque. It comes in five shades, just like RelyX Veneers Cement. The inorganic fillers are ytterbium trifluoride and spheroid mixed oxide.
Dental Composites
Dental composite resins are most commonly composed of Bis-GMA and other dimethacrylate monomers, such as TEGMA, UDMA, HDDMA. They also contain a filler material such as silica. When properly bonded to the tooth structure, it is the most conservative dental material available. There are principally three categories of dental composites:
- Microfills
- Microhybrids
- Nanofills
Microfills render the most aesthetic and natural-looking direct dental restorations. They have the smallest average particle size (0.04 µm) of all available direct composite resins and can therefore be polished to a high luster. Microfills keep their luster more than microhybrids or nanofills and are more stain and plaque resistant, which contributes to a healthy gingival tissue. Their high refractive index leads to the most realistic translucency. The refractive index of a material is a dimensionless number that describes how light propagates through that medium. The refractive index for vacuum is 1, for a diamond it is 2.4. The refractive index of enamel is 1.6. This may vary slightly from individual to individual. Microfills are in the same range.
However, microfills are less filled than other composite resins. They are therefore used in layering techniques placing as the enamel layer above a stronger dentin layer composite, such as microhybrid or nanofill composite
Microhybrids most closely approximate the physical and optical properties of the dentin of natural tooth structure. Just like in a natural tooth, they are "tough" (a physical property) and more opaque than the enamel layer. They are often combined with microfills that are used for the more translucent superficial layers, mimicking the dental enamel. The larger particle size of microhybrids, compared to nanofill and the microfill composites, results in higher strength and toughness. Microhybrids are the most opaque of the composite types described here. They are therefore indicated for masking stained tooth surfaces when considerable color changes are desired.
Hybrid composite materials can be divided into coarse, fine, and micro hybrids, either homogenous and inhomogeneous. Their matrices consist of
- methacrylates
- ormocers
- compomers
- silorane-based.
Microhybrids are less polishable and more difficult to adapt to their interfaces with the tooth structure. They wear faster than microfill resins. This is why microhybrids are ideally combined with microfills as the substructure in areas that require high strength and significant color changes.
Nanofill composites combine conventional fillers with nanoparticles to combine both, strength and aesthetics, in one material.
- Completely nanofilled resins contain nanometer-sized particles throughout the resin matrix.
- Nanohybrids, on the other hand, consist of larger particles surrounded by nanometer-sized particles.
As previously mentioned, nano-hybrids contain nanometer particles combined with larger particles, which leads to a strength similar to classical hybrids and higher polishability, as for microfill resins. Microfillers contain particles that are smaller than 1 micron, while nanofillers contain particles that are smaller than 0.1 micron.
IPS Empress and E.max
IPS Empress and E.max glass ceramics are used for VENEERS and CROWNS.
Their physico-mechanical properties such as modulus of elasticity, hardness, and coefficient of thermal expansion are very close to natural enamel. Glass may be defined as a rapidly undercooled liquid with an amorphous, noncrystalline structure. When glass melt is cooled slowly, crystals develop. Glass ceramics are produced from raw glass by controlled crystallization. One or more types of crystals embedded in one or more vitreous phases result from this "ceramming" process. IPS Empress and E.max consist of crystals and a vitreous phase. The glass matrix merely forms a putty between abundant leucite crystals.
Different factors account for the improved mechanical properties of these materials. One factor is the stress which is set up in the vitreous phase as a result of the high shrinkage of the leucite crystals. Secondly, the leucite crystals with a mean diameter of 3 micrometer are believed to stop the propagation of micro-cracks within the glass matrix. The wear of IPS Empress glass ceramics is in range of enamel. As a result of its fine-grain structure, the glass ceramic abrades the antagonist (opposing dentition) enamel not more than natural enamel.
For more information about porcelains, see also the page explaining porcelains in more detail.
Porcelain-fused-to-metal Crowns and Bridges
These restorations have an invisible metal core, which is covered by a layer of feldspatic porcelain. Usually these restorations are not aesthetic as all-porcelain (glass ceramic) restoration, but certain conditions, such as root-canal-treated teeth and long-span bridges, require the additional strength derived from the metal core.
What are Ceramics and Porcelains?
Ceramics are defined as man-made solid objects formed by nonmetallic and inorganic raw materials that are baked at high temperatures. The traditional porcelain is composed of three naturally occurring minerals: pure white clay, silica, and feldspar.
The basic components of dental porcelain are silica and feldspar. Additional components are aluminum oxide as well as pigments and opacifying agents, depending on the application. Only denture teeth contain clay as the third basic component of traditional porcelain.
All baked dental porcelains contain small crystals (leucite and/or alumino-silicate crystals) that are embedded in a silicate matrix. The relative amount of crystals and glass depend on the specific porcelain. Leucite, a reaction product of potassium feldspar and glass, is a particularly important component of dental porcelain, because it affects its optical properties, thermal expansion, strength, and hardness.
Until recently, all-porcelain restorations were used with caution because of two inherent problems: the risk of brittle fracture and the abrasive wear of opposing tooth structure. Brittle fracture is generally attributed to the rapid, uninterrupted propagation of cracks, usually beginning at a flaw in the ceramic. This failure is often initiated at the internal surface. Aluminous oxide has been added to increase the strength of dental porcelains. However, aluminous crowns fit very poorly due to the shrinkage during baking procedures. Therefore, dental ceramics fused to metal substrates have been the preferred treatment modality.
Metal bases affect the aesthetics of porcelain by decreasing the light transmission through the restoration and by creating metal-ion discoloration. In addition, some patients may have allergic reactions or other sensitivities to metals. These drawbacks have prompted the development of new all-ceramic systems that do not require metal, yet have the high strength and precision fit of ceramometal systems. Among the systems available today are the powder-slurry ceramics (e.g. Optec HSP, Duceram LFC), castable ceramics (e.g. Dicor), machinable ceramics (e.g. Cerec Vitablocks, Dicor MGC), infiltrated ceramics (e.g. In-Ceram), and pressable ceramics (e.g. IPS Empress, IPS E.max, Optec Pressable Ceramic).
IPS Empress is a heat-pressed glass ceramic that has superior mechanical properties for several reasons. The high shrinkage of leucite crystals creates compressive stress in the vitreous phase, which prevents the development of surface cracks. The randomly oriented leucite crystals are tightly packed in the vitreous phase and stop the propagation of micro-cracks. The combination of heat pressing, initial firing, and stain and glaze of the veneers creates an additional 50% increase in strength. This higher cohesive strength and fracture toughness allows for thicker areas of porcelain with a lesser risk of fracture. Unbonded glazed IPS Empress has a flexural strength of 215 MPa compared to 71 MPa of feldspatic porcelain, 114 MPa of Dicor, 167 MPa of Optec HSP, and 419 MPa of In-Ceram.
IPS Empress is bonded to dentin with a resin cement after conditioning of the surfaces of both the restoration and the prepared tooth. This further increases its fracture resistance significantly and reduces microleakage. The occlusal wear of IPS Empress is in the range of enamel due to its fine-grain structure.
All-porcelain restorations allow direct light to penetrate. The amount of scattering versus transmission of light depends on the chemical composition of the porcelain's glass matrix, the size and structure of the crystalline phase, and the processing technique. Light penetration adds a translucency to the restorations that is comparable to natural teeth even under compromised light conditions, since there is no metal substructure that interferes with the transmission of light. The transillumination quality also improves the natural pale-pink appearance of the adjacent marginal gingiva.
References:
Triolo PT et al. Shear bond strengths of composite to dentin using six dental adhesive systems. Operative Dentistry 1995, 20(2); 46-50.
Wilder AD et al. Bond strength of conventional and simplified bonding systems. Am J Dentistry 1998, 11(3); 114-117.
Boksman L et al. Adhesives: Newer is Not Always Better - Part 1 - Latest-generation adhesives often do not measure up to their predecessors in bonding strength and durability. Inside Dentistry 2012, 8(2); pageless at dentalaegis.com.
Arrais CA, Giannini M. Morphology and thickness of the diffusion of resin through demineralized or unconditioned dentinal matrix. Pesqui. Odontol Bras. 2002;16(2); 115-120.
Hashimoto M et al. The effect of hybrid layer thickness on bond strength: demineralized dentin zone of the hybrid layer. Dent Mater. 2000;16(6); 406-411.
Christensen GJ. Bonding agents: Is convenience overriding strength? Clinician’s Report reprint from June 2010. Dental Economics. 2010; 3(6); 1-3.
De Munck J et al. Four year water degradation of total-etch adhesives bonded to dentin. J Dent Res. 2003;82(2); 136-140.
Melo RM et al. Bond Strength of Two Resin Cements on Dentin Using Different Cementation Strategies. J Esthetic and Restorative Dentistry 2010; 22(4); 262-8.
Bisco Canada. All Bond 2 Information Sheet.



