Porcelain Veneers for Stained Teeth with Gummy Smile
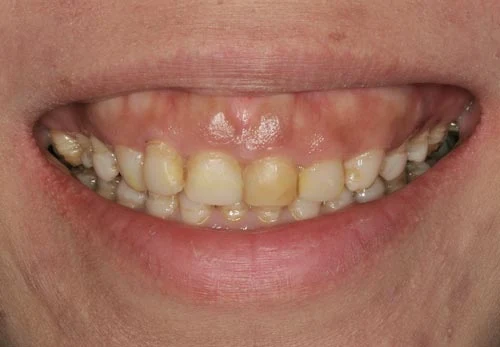
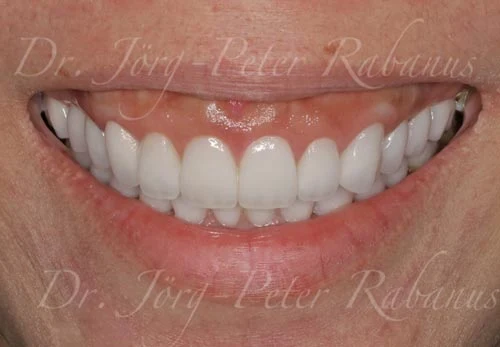
Cosmetic dentists are confronted with a wide spectrum of oral conditions that affect the aesthetic appearance of a smile. Most potential patients who are looking for a smile makeover believe that porcelain veneers will solve their aesthetic concerns. However, in most cases, it is not that straightforward.
You can find many dental conditions that are described in this website. Find the link that applies to you in the menu on the left or click here:
While any of these concerns of potential cosmetic dental patients are well founded, their treatment by way of smile makeovers is not one-dimensional. The oral cavity is a three-dimensional multi-functional space that needs to be thoroughly understood by the treating cosmetic dentist. Some functional aspects were outlined in the discussion of comprehensive smile makeovers.
The images above represent a more complex challenge for a cosmetic dentist that cannot be addressed by simple placing porcelain veneers.
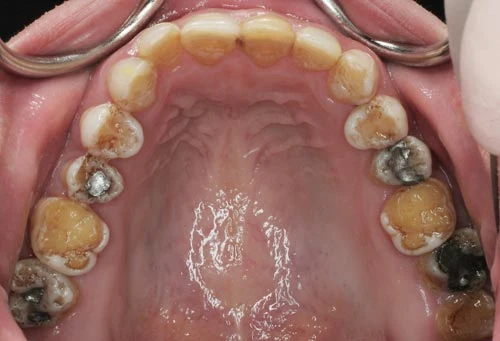
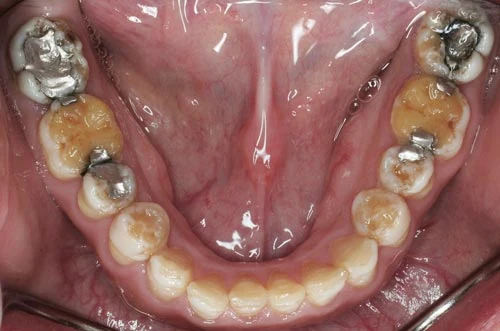
Looking at the occlusal surfaces of these upper and lower teeth, it becomes immediately apparent that almost all enamel is missing. This has a big impact on the way this patient bites and chews. The reader shall be reminded of the amazing act of nature regarding the development of teeth in two opposing jaws and the development of dental cusps via intricate interactions of highly specialized and differentiated cranial cells. It never seizes to inspire me with awe how these cranial cells execute their individual functions without losing the big picture. At the end, upper and lower teeth perfectly fit against each other despite have grown in seperate jaws.
While this website primarily serves as a guide for persons who look for information about cosmetic dentistry, the biological implications merit consideration. Every structure of the skull is highly specialized, yet interacts intricately with the other. The common links are found in the embryological development and migration of the cell lines that are responsible for the cranial structures. As an example, cells taking part in the development of the temporomandibular joints have the same origin as the cells responsible for tooth form and location (1).
As much as cosmetic dentists are primarily clinicians, only an understanding of craniofacial devlopment will complete the apprehension of the functional and aesthetic construct of a human face (2).
How does the comprehensive understanding of facial development and oral function impact the treatment planning for a smile makeover?
Loss of tooth structure is one of the main reasons why people seek cosmetic dentistry. Most of them believe that a simple set of porcelain veneers will address any type of tear and wear of teeth. However, front teeth cannot be isolated from the function of their companions, the back teeth. In fact, front teeth are only a small functional component of the face. Yes, upper incisors have a huge social impact - a beautiful smile goes a long way in life. But teeth of the smile zone are intimately intertwined with all structures of oral function, such as lips, tongue, periodontal tissues, cranial muscles, and temporomandibular joints. Cosmetic dentists who are familar with the interrelationships of the neuronal hardwiring among these structures understand how, for example, periodontal sensory inputs interact with the entire masticatory system (3-15).
Teeth cannot be appraised without their contextual environment of the oral cavity, the face, and the skull.
The utilization of facebows establish reference to facial landmarks, such as the line that connects the pupillae of both eyes. Photographs with facebow in place become powerful tools to communicate to the dental technologists vital landmarks for the execution of the smile design (16,17).
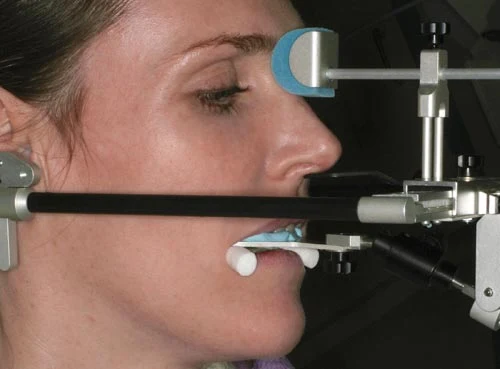
A meticulous documentation of the facial framework that a new smile is designed for prevents unnatural outcomes. The orientation of the smile line is one of the most fundamental underpinnings to ensure the harmonious integration of a smile makeover.

Another important point of reference is the location of the mandibular joint as it relates to the base of the skull. Numerous cranial neuromuscular feedback mechanisms collectively guide the temporomandibular joint (TMJ) into its position against the articular disk. In fact, the content of the articular capsule and the surrounding attached soft tissues are the only means by which the mandible is connected to the base of the skull. Hence, the mandibular teeth are connected to the maxillary teeth indirectly via a disk and a soft-tissue assembly, which makes a finely tuned positioning system indispensible.
The cranial positioning system obtains its input from receptors within the periodontal ligament, cranial bones, muscles, tendons, and joints. This coincides with a plethora of possible disturbances among the feedback mechanisms of the masticatory system. This may create a confusion of signals that may lead to bruxing or grinding. The ensuing premature and uneven wear of teeth will add to the confusion of the system and may contribute to the aggravation of dysfunctional patterns, completing the vicious cycle. A meticulous analysis of existing dental wear is therefore indispensible when planning a smile makeover.
How an individual "cranial positioning system" impacts a smile design, from porcelain veneers to comprehensive oral rehabilitation:
The dental deterioration presented above has a different and unique origin: defective dental enamel. The reasons may be genetic, such as Amelogenesis Imperfecta. In this case, the dental hypoplasia appears to be caused by tetracycline (18-21). The deterioration of dental enamel at the contact surfaces between maxillary and mandibular teeth challenges the feedback mechanisms of the cranial positioning system, which may lead to dysfunction and additional premature wear of the dentition.
When the patient appeared at my office, she considered getting porcelain veneers to address her aesthetic concerns without being aware of the underlying causes and hidden structural damages that needed to be analyzed prior to creating a treatment plan for a smile makeover. It could be assumed that the temporomandibular joint was not in its "home" position when upper and lower teeth met.
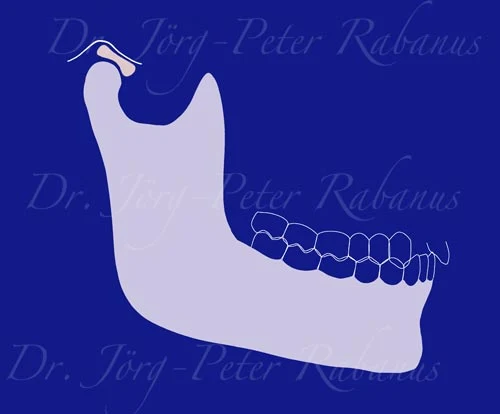
Healthy, well-aligned, and unworn teeth help their temporomandibular joints to remain in their "home" position when upper and lower teeth meet. Genetic code and epigenetic mechanisms lead to a proportionate structural layout of all involved anatomical elements of the masticatory system with a total harmony of function. All sensory inputs of this system are compiled, assessed, and correlated in specialized networks of the central nervous system to ensure a coordinated motoric function.
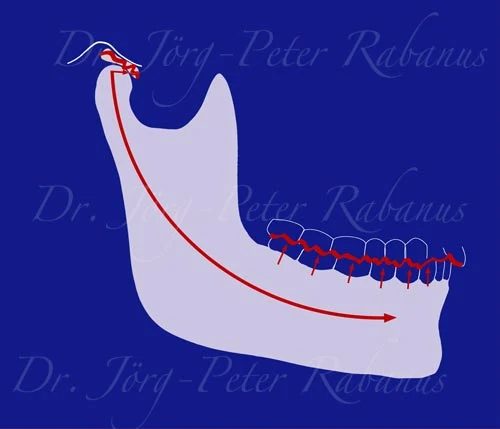
Teeth that have suffered damage and deterioration due to various mechanisms, such as bruxism, acidic erosion, or enamel dysplasia, may not contribute anymore to their temporomandibular joints' "home" position when upper and lower teeth meet. Dental cusps have lost their form and outline that was intimately entwined with all oral structures by a coordinating genetic code and epigentic mechanisms. Hence, each time when damaged teeth connect, mandibular joints may get displaced out of their physiological relationship against the base of the skull and their surrounding tissues.
The consequences may be detrimental, leading to an imbalance of the forces developed by the masticatory system, possibly triggering a vicious cycle that leads to an accelerated breakdown of tooth structure, the articular assembly of the joints, and other oral structures. Premature aging of the lower face or cosmetic dental concerns of the individual might be the consequences.
To be continued . . .
References:
1. Chai Y et al. Fate of the mammalian cranial neural crest during tooth and mandibular morphogenesis. Development, 2000, Vol. 127: 1671-1679.
2. Minoux M et al. Molecular mechanisms of cranial neural crest cell migration and patterning in craniofacial development. Development, 2010, Vol. 137: 2605-2621.
3. Trulsson M et al. Encoding of tooth loads by human periodontal afferents and their role in jaw motor controls. Progress in Neurobiology, 1996, Vol. 49: 267-284.
4. Türker KS et al. The role of periodontal mechanoreceptors in mastication. Arch Oral Biol, 2007, Vol. 52: 361-364.
5. Brinkworth RS et al. Response of human jaw muscles to axial stimulation of the incisor. J Physiol, 2003, Vol. 547: 233-245.
6. Sensory and motor function of teeth and dental implants: A basis for osseoperception. Clinical Exp Pharm Physiol, 2005, Vol. 32: 119-122.
7. Shi L et al. Requirement of occlusal force for maintenance of the terminal morphology of the periodontal Ruffini endings. Arch Histol Cytol, 2005, Vol. 68 (4): 289-299.
8. Brinkworth RS et al. Response of human jaw muscles to axial stimulation of a molar tooth. Exp Brain Res, 2004, Vol. 159: 214-224.
9. Johnsen SE et al. Forces applied by anterior and posterior teeth and roles of periodontal afferents during hold-and-split tasks in human subjects. Exp Brain Res, 2007, Vol. 178: 126-134.
10. Trulsson M et al. Directional sensitivity of human periodontal mechanoreceptive afferents to forces applied to the teeth. J Phys, 1992, Vol. 373-389.
11. Jacobs R et al. From osseoperception to implant-mediated sensory-motor interactions and related clinical implications. J Oral Rehab, 2006 Vol. 33: 282–292.
12. Trulsson M et al. Force encoding by human periodontal mechanoreceptors during mastication. Arch Oral Biol, 2007, Vol. 52: 357-360.
13. Brinkworth RS et al. Jaw movement alters the reaction of human jaw muscles to incisor stimulation. Exp Brain Res, 2005, Vol. 164: 165-176.
14. Maeda T et al. The Ruffini ending as the primary mechanoreceptor in the periodontal ligament: its morphology, cytochemical features, regeneration, and development. Crit Rev Oral Biol Med, 1999, Vol. 10(3): 307-327.
15. Trulsson M et al. Sensory-motor function of human periodontal mechanoreceptors. J Oral Rehab, 2006, Vol. 33: 262–273.
16. Olitsky J. Seven worst violations of smile design. Inside Dentistry, 2015, Sept.: 60-68.
17. Sanders KS et el. Dentist-Laboratory Communication About a complex Case. J Cosm Dent, 2010, Vol. 26(2): 108-117.
18. Witkop CJ et al. Hypoplasia and Intrinsic Staining of Enamel Following Tetracycline Therapy. JAMA, 1963, Vol. 185(13): 1008-1011.
19. Fleming P et al. Staining and hypoplasia of enamel caused by tetracycline: case report. Pediatric Dentistry, 1987, Vol. 9(3): 245-246.
20. Kashyap AS et al. Discolouration of permanent teeth and enamel hypoplasia due to tetracycline. Postgrad Med J, 1999, Vol. 75(8): 772.
21. Sanchez, AR et al. Tetracycline and other tetracycline-derivative staining of the teeth and oral cavity." Int J Dermatology, 2004, Vol. 43: 709-715.



